During the MEDLIFE Mobile Clinic in Panama this summer, student volunteers were shocked by the large number of patients who came in with ulcers on their skin. The doctor who worked with us on the clinic explained that these were symptoms of Leishmaniasis — a disease which is rampant in the jungle and mountainous areas of Panama.
Leishmaniasis is transmitted through the phlebotomine sandfly, which thrives in the intertropical regions of the world and threatens the 350 million people living in these areas. There are an estimated 12 million current cases of leishmaniasis worldwide, with another 1.5 to 2 million people infected annually. Around 88,000 people die each year from the disease.
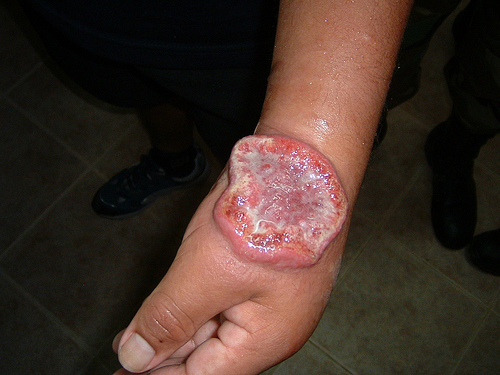
Patients with mucocutaneous leishmaniasis develop lesions similar to those with cutaneous leishmaniasis, but the lesions occur in the mucous membranes rather than on the skin of the patient. These lesions generally occur between 1-3 months after the initial infection; however, there have been cases where it has been decades after the initial bite that the patient shows symptoms.
In some cases, the mucotaneous lesions are the first symptoms a patient will express; other times the patient will first have cutaneous lesions followed by mucotaneous sores that develop later in the course of the disease. The lesions can lead to partial or total destruction of the nose, mouth and throat. They also may cause nasal obstruction and bleeding. Not only is this very painful for the patient, but it can also lead to facial disfigurement. Often those who suffer from mucotaneous leishmaniasis are ostracized completely from their communities.
The most serious form of the disease is visceral leishmaniasis. In some regions of the world this is known colloquially as Kala-Azar. Sufferers of this form of the disease have fever, weight loss, anemia, swelling of the spleen and liver, and a darkening of the skin. If untreated, visceral leishmaniasis has a 75-95% mortality rate, although it this rate may reach 100% in developing countries.

One of the largest burdens of this disease is the social ostracization that many leishmaniasis patients face due to disfiguring scars. As the importance of community support is heightened in poor and rural areas, these social ramifications can be as serious for patients as their physical symptoms.
Though there are several medications which treat all three forms of Leishmaniasis, access to this medicine is severely limited for those without adequate health care coverage. If the disease is caught early, cure rates are incredibly high. Yet, as the disease progresses, it can harm the immune system, and eventually cause death.
During our Mobile Clinics in Panama, it became clear that many of our patients suffered from this disease. Seeing so many patients with Leishmaniasis underscored the importance of increasing medical care access in these incredibly rural communities so that people can get the treatment they need for such a common and treatable disease.
Post by Lisa Berdie, MEDLIFE Summer Intern in Panama
